Mammograms Aren't as Great as You Think
By:
October is breast cancer awareness month, which for many women is a reminder to get mammograms — x-rays of breast tissue that can detect early indicators of cancer. But recent research suggests that there are a few important things to keep in mind: not only can mammograms vary wildly in cost, but researchers also now say that Americans pay too much for mammography technology that is largely ineffective and in some cases more dangerous to women's health.
Mammograms are in many cases crucial for catching early signs of breast cancer, which could otherwise quickly spread to other parts of the body and become deadly. But a growing body of evidence has many—scientists, medical professionals, and patients—second guessing a method of cancer screening once thought to be infallible. The most recent research, it turns out, only builds on what some in the field have suspected for years.
Here are three reasons people are reconsidering mammograms.
1. Technology used in 90 percent of mammograms is ineffective
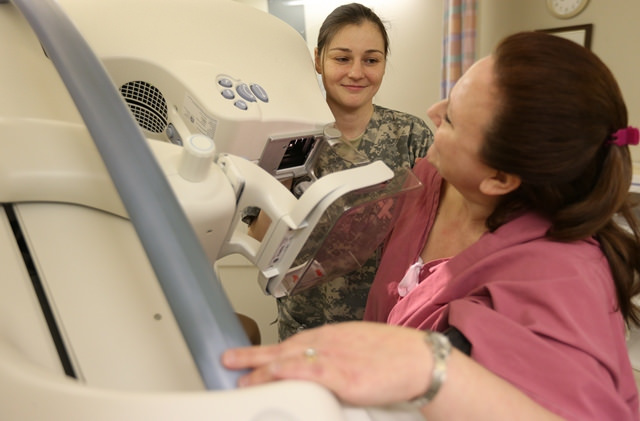 Army Medicine / Flickr - flickr.com
Army Medicine / Flickr - flickr.com
According to a recent study that surveyed more than 625,000 digital mammograms spanning 66 different facilities, the high-tech screening technology used in most procedures makes no improvements to the accuracy of how often cancers were detected, how often they were missed, or how often cancers were mistakenly labeled. That technology is known as computer-aided detection, or CAD. It adds markings to breast tissue scans to help highlight problem areas, but the study found that radiologists correctly identified cancer more often without the use of CAD.
In an accompanying editorial, the study's authors pointed out that Medicare reimbursed health care centers for CAD-aided mammography procedures, which they said costs the U.S. at least $400 million each year using conservative estimates. The technology was first approved under dubious circumstances by the U.S. Food and Drug Administration, but was not widely used until 2002, when the Centers for Medicare and Medicaid Services adopted reimbursement.
"This is a very important study from the perspective of establishing whether or not people are going to change practice around reimbursement," Diana S.M. Buist of the Group Health Institute, which helped conduct the study, told ATTN:. "Unfortunately, this is not the first and will not be the last diffusion of technology with reimbursement incentives that are provided in the absence of evidence."
2. Some say mammograms cause emotional turmoil—and expensive false alarms
 Caitlin Regan / Flickr - flickr.com
Caitlin Regan / Flickr - flickr.com
The question of when and how often women should start getting mammograms is decades old. In 2009, the U.S. Preventive Services Task Force raised the age at which they recommend women start getting mammograms from 40 to 50. But questions regarding how many woman have been harmed by mammograms have only begun emerging in recent years.
A new story in Mother Jones, for example, looks at some of the dangers that can come from the procedure's propensity to "overdiagnose" things that look like cancer, but may not end up acting like cancer in the body. Those misdiagnoses can feed into a culture of fear, where uncertainty over the meaning of biopsy results flourishes. In the best cases, that means being overly cautious about abnormal tissue formations. But in the worst, it could mean expensive, lengthy, dangerous, and terrifying procedures which could involve losing one or both breasts over formations that have a small chance of turning into cancer.
Mother Jones writes:
"Mammograms do help a small number of women avoid dying from breast cancer each year, and those lives count, but a 2012 study published in the New England Journal of Medicine calculated that over the last 30 years, mammograms have overdiagnosed 1.3 million women in the United States. Millions more women have experienced the anxiety and emotional turmoil of a second battery of tests to investigate what turned out to be a false alarm."
3. Expanding treatment options
Mammograms can turn up what's often called Stage 0 breast cancer—ductal carcinoma in situ, or DCIS. But new attitudes among patients and doctors alike favor treating the still-not-fully-understood DCIS with cautious monitoring, not a barrage of radiation, surgery, or mastectomies. In what's called active surveillance, patients who have the earliest stages of cancer can take a gentler route that seeks to closely monitor what might never turn into full-blown cancer at all. One patient highlighted in a recent Time article, opted to take an estrogen-blocking drug and go in twice-a-year for mammograms and MRIs—eight years ago.
"Our two greatest challenges...are figuring out better treatments for the 40,000 women who die of breast cancer every year, and at [the] same time, figure out who, on the other end of the spectrum, is getting exposed to needless toxicity," the director of breast oncology at Dana-Farber/Brigham and Women's Cancer Center, Dr. Eric Winer, told Time.
The question here is not necessarily whether to doubt the efficacy of mammograms—they are, after all, an essential tool for highlighting potential problems and subsequent deadly outcomes. But the medical establishment is showing signs of slowly moving away from treating the earliest forms of cancer in the same manner as the fully fledged sort. Frequent, cautious observation, the logic goes, can be a smarter approach than overtreatment and overdiagnosis.
