Sexual Health Questions Men Should be Asking

By:
Over the past week we’ve been hearing a lot about women’s health—in part due to the political attempt to defund Planned Parenthood.
Women aren't the only ones who need to take care of their sexual health—and they aren't the only ones who use Planned Parenthood. Men are 24 percent less likely than women to have visited a doctor (of any kind) in the past year, which includes making an appointment to address their sexual health.
If something seems off—abnormal, non-functioning, painful—it’s important to have the issue evaluated and treated by a medical professional ASAP. But, even if the male body feels like it’s running smooth and sexy, there are some critical questions men should be aware of asking for the best chance at being their healthiest best.
1. STIs: Should I get screened?
The short answer is, if you’re sexually active, yes. Sexually Transmitted Infections (STIs) are an incredibly common occurrence; more than half of all Americans will contract at least one STD/STI at some point in their lives. In fact, one out of two sexually active individuals will contract an STI before age 25. STIs are passed between people during sexual contact. Many infections often don’t cause symptoms; medically speaking, when infections cause symtoms they're called diseases (Sexually Transmitted Diseases).
STIs run the gamut from Chlamydia to Herpes to molluscum contagiosum. The scary sounding infections can be managed and many can be cured with proper treatment. However, the first step is to get tested. Different tests examine for different infections and it’s necessary you ask for specific tests.
While not an STD, men can also experience yeast infections, caused by a build up of yeast. Men may notice redness and irritation in their genitals as contraction symptoms.
Some states—Washington, California, Minnesota—make it incredibly easy and comfortable to get tested. You can order STD test kits for at-home usage (with clear instructions of course), which test for Chlamydia and Gonorrhea. Tester then mails the samples back in a pre-paid package. Request a test at a local Planned Parenthood center or private health care provider.
2. Have I been checked for testicular cancer?
Testicular cancer is common in young men ages 20 to 34—over half of case occur in this age range. The risk factors can vary but include family history, HIV, and a genetic condition called Klinefelter's syndrome, which can lead to underdeveloped testicles. Often painless, save for discomfort, the most common symptom of this cancer is swelling or a lump in the testicles. Men should perform a testicular self-exam monthly and if a hard, smallish (pea-sized) lump is found or a testicle seems enlarged, contact a healthcare provider without delay.
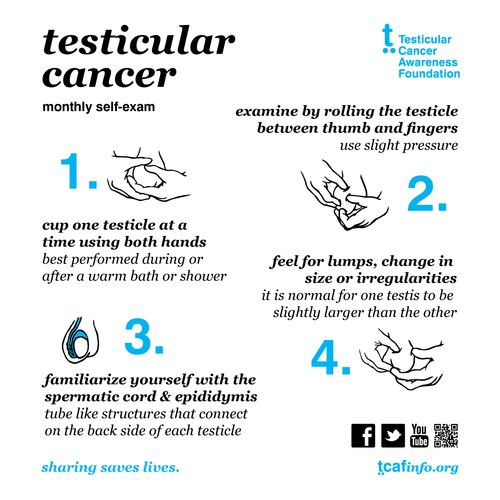 Testicular Cancer Awareness Foundation - testicularcancerawarenessfoundation.org
Testicular Cancer Awareness Foundation - testicularcancerawarenessfoundation.org
3. Should my testosterone levels be checked?
Testosterone is the king of male sex drive and when levels decrease—as they naturally do, especially with men, about one percent a year after age 30—it affects sexual and reproductive health as well as fat distribution and muscle strength maintenance.
Indicators of low testosterone, also known as hypogonadism, vary from erectile dysfunction, increased breast size, fatigue, depression, irritability, lack of concentration, loss of body mass, loss of height, and low libido. Low levels of testosterone drop slower than say estrogen during menopause, so it can be more difficult to detect. If symptoms occur and persist it’s time to make a doctor’s appointment. Levels can be brought closer to normal through an artificial version of the hormone via pills, implants, gels, and patches.
4. What birth control options do I have?
The word “birth control” tends to bring condoms and rows of white pills in pink packaging to mind, but soon there may be many more options for sexually active men other than the condom. (Also, if you have any questions on condom use, please talk to a doctor. ATTN: has reported that condom use fluctuates by age.)
Research is currently being conducted on options including gels, implants (like the male counterpart to Nexplanon) and pills for men. Such future options may assist in balancing out the physical and financial side effects of birth control, which has for a long time been utilized and created for women. There is also the current option of the vasectomy, which is intended to be permanent as the sperm-transporting tubes are cut or blocked. While the no sperm, no pregnancy set-up may sounds like a great idea at first, mull it over with a doctor first as it can be a life-changing decision.
There are many more questions for men to consider regarding their sexual health including what is erectile dysfunction (ED) and how to improve libido. Know that sexual health is piece of the full picture of general health. For example, men with erectile dysfunction are more likely to have heart disease and heart attacks than those that do not have ED. For the sake of long-term health, schedule an appointment and talk to a doctor about current sexual health issues and preventative measures.
