How Medicaid Rescued This Man From Opioid Addiction

By:
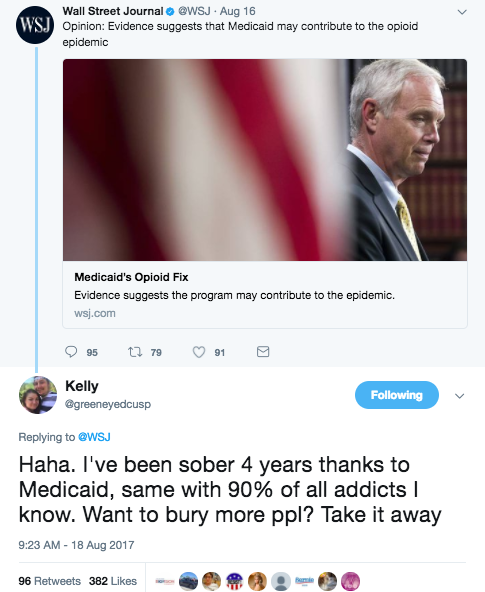
Last week, Kelly came across an opinion piece from The Wall Street Journal editorial board that laid partial blame for the nation's opioid epidemic on Medicaid expansion. It was an absurd suggestion, he thought, considering how Medicaid saved his life.
 Twitter - twitter.com
Twitter - twitter.com
Kelly, who asked that we use only his first name, struggled with opioid addiction for seven years, abusing potent painkillers like OxyContin and eventually, heroin. It wasn't until he found himself hospitalized in 2013—facing a $40,000 medical bill because he was uninsured—that his doctors helped him enroll in Medicaid and got him into treatment.
Now four years sober, Kelly credits Medicaid expansion under the Affordable Care Act (ACA) for his recovery. He told ATTN: he was "able to get access to a ton of resources" that weren't "even in the realm of possibility because of how expensive [they were]" without health insurance.
I asked where he thought he'd be today without Medicaid. "Honestly? If not dead, definitely still using," he said. Instead, the 29-year-old is back at school studying linguistics, with hopes of becoming a teacher and mentoring people going though addiction.
 Flickr - flic.kr
Flickr - flic.kr
Nearly 2 million Americans can relate to Kelly's story. That's how many people have received treatment for substance abuse and mental health issues through Medicaid since its expansion, according to a 2017 study from Harvard Medical School and New York University.
The types of addiction treatment services covered through Medicaid range vary depending on what state you live in, but the most common examples include outpatient mental health counseling, partial hospitalization programs, which include group and individual therapy sessions, and "community treatment" services, which include intensive therapy and skills training.
These programs are undoubtedly helpful for some opioid users, Dr. Andrew Kolodny, co-director of opioid policy research at Brandeis University, told ATTN:. But he noted that Medicaid expansion has proven particularly essential through its coverage of addiction treatment drugs like buprenorphine, a drug that helps users wean off more dangerous opioids.
"The first-line treatment for opioid addiction is treatment with buprenorphine—and in some cases, methadone maintenance," Kolodny said. "For people who are able to recover without needing to be on buprenorphine or methadone maintenance, that's great—that's better than being stuck on another drug. But most people who are opioid addicted can't recover that way. They wind up relapsing and overdosing."
He added, "There are many people who, because of Medicaid expansion, their Medicaid is paying for their buprenorphine prescriptions."
 Flickr/frankieleon - flickr.com
Flickr/frankieleon - flickr.com
For his part, Kelly said he benefited most from "access to a therapist and psychiatrist" who helped him "fix the underlying issues."
"But also access to suboxone [buprenorphine]," he said. "A lot of people not in the world of addiction [consider it] just a replacement for opiates, but that simply isn't true. People getting off of opiates without a suboxone or methadone to taper off are much more likely to fail and not get sober."
Like access to addiction treatment, access to treatment drugs has also significantly increased in the years since the ACA took effect. From 2011 to 2016, Medicaid spending on these prescriptions (e.g. buprenorphine, naltrexone, and naloxone) grew 136 percent, according to a recent report from the Urban Institute.
Statistics illuminating how Medicaid expansion has expanded access to these life-saving services raise questions about the "intriguing evidence" the Journal cited in its op-ed.
 AP/John Dixon - apimages.com
AP/John Dixon - apimages.com
The Journal cited data obtained through the office of Sen. Ron Johnson (R-Wisc.), which indicated that opioid overdoses rates were higher in states that accepted Medicaid compared to non-expansion states. It also supported the senator's theory that the health care program had "created a perverse incentive for people to use opioids, sell them for large profits, and stay hooked."
"The argument doesn't really make sense," Kolodny said. "We know that this is an epidemic caused by overprescribing of opioid pain medicine. You could make a case that people who have no access to doctors would be less likely to become opioid addicted—and I do think you could make a fair argument—but this has nothing to do with Medicaid expansion."
Kolodny continued:
The opioid addiction epidemic began in 1996—and Obama's Medicaid expansion began in 2010. By 2010, we were well into the epidemic, very deep into it. By 2010, the [Center for Disease Control and Prevention] was already calling this an epidemic and calling it the worst drug addiction epidemic in U.S. history before there was any Medicaid expansion. The timing doesn't make any sense.
It should be said that Johnson's theory sits well outside of mainstream thinking on Capitol Hill. But it does echo an argument that has been used in health care debates over the past few months, with Republicans downplaying the consequences of Medicaid rollbacks that have been proposed in various GOP bills.
Kelly said he's watched lawmakers push for Medicaid rollbacks with "absolute horror."
 AP/J. Scott Applewhite - apimages.com
AP/J. Scott Applewhite - apimages.com
"I have lost more friends than I can count to this disease, and I know if they had access to some of those resources, maybe they'd have a second shot like I got," he said. "If this administration cared about this opiate epidemic, they'd allocate resources to the institution helping most: Medicaid," he said.
"This is not hyperbole. More people will die if these resources get stripped from addicts."
