White House Cracks Down On Birth Control Mandate

By:
In response to reports that insurers were violating the Affordable Care Act's (ACA) free birth control coverage rule, the White House has warned insurance companies that they must provide all forms of approved contraceptives to users at no cost or co-pay charge. The National Women’s Law Center and the Kaiser Family Foundation recently drew attention to the issue by publishing separate investigations that revealed not all insurance companies are following the law. Now the Obama administration is reiterating that insurance plans have to cover all forms of birth control approved by the U.S. Food and Drug Administration (FDA).
“Insurance companies have been breaking the law, and today the Obama administration underscored that it will not tolerate these violations,” Gretchen Borchelt, vice president of the National Women’s Law Center, told the New York Times. “It is now absolutely clear that all means all — all unique birth control methods for women must be covered.”
The Kaiser study, which observed and interviewed 20 insurers in five different states, showed many insurance companies were engaged in "reasonable medical management," meaning insurers barred access to certain kinds of birth control when they believed there was a cheaper form for women to use. According to the new ACA standards, this is illegal. The Kaiser report concluded that one company didn't provide coverage for the NuvaRing, which has been FDA-approved since 2001. An insurance company in the study said it covers the birth control pill in full but requires "cost-sharing for the NuvaRing, which has the same chemical composition," according to the Kaiser report.
The research found that some plans reduced accessibility to patches and the ring, pushing users to take the birth control pill instead. One insurer said users must "show medical necessity on why oral contraceptives are not suitable before they will cover the NuvaRing." The study also found that some companies did not cover Skyla, an intrauterine device (IUD) that lasts up to three years, but all covered Mirena, a longer-lasting IUD.
"It is past time for insurers to adhere to the law and stop telling women that their chosen method isn’t covered or that they must pay for it," Borchelt said in a statement. "We welcome the Administration’s guidance and know it will go a long way to improve the health and economic well-being of women and their families."
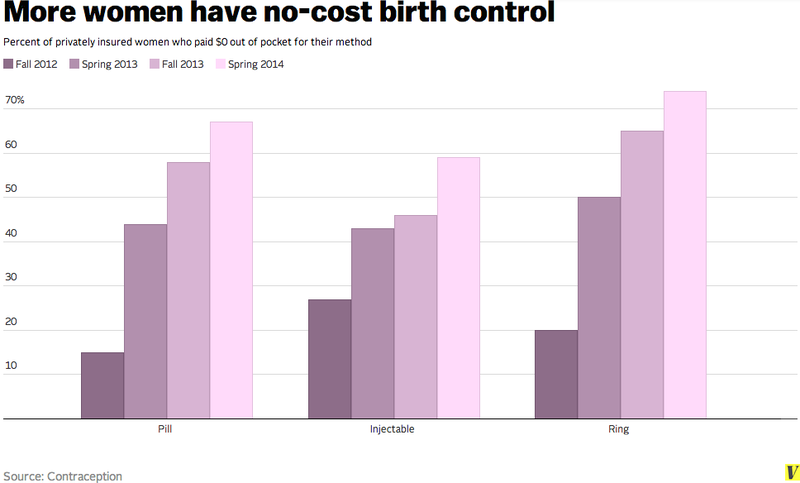
Last year, the journal Contraception found that nearly 70 percent of privately-insured women received free birth control pill coverage, a 15 percent increase from 2012.
 Vox - vox.com
Vox - vox.com
As pointed out by Vox, the percentage of women who do pay for birth control can likely be attributed to grandfathered insurance plans, which are exempt from many ACA policies because they predate the law. However, grandfathered plans are uncommon because insurers must forfeit their grandfathered privileges when they make drastic changes to plans like decreasing benefits or increasing costs for users. Grandfathered plans are health policies purchased on or prior to March 23, 2010, when the ACA went into law. They only make up 26 percent of all health plans, according to a 2014 Kaiser Family Foundation report.
In addition to covering contraceptives, the White House also said insurers are required to cover genetic counseling and screening to women who have a family history of ovarian or breast cancer. Specifically, it said, insurers must cover testing for mutations in the BRCA1 and BRCA2 genes, which can increase a woman’s risk of developing breast or ovarian cancer.
Katie Hill, a spokeswoman for the Department of Health and Human Services, told the Times that insurers also have to "cover preventive screening, genetic counseling and genetic testing without cost-sharing when an individual has a family cancer history associated with increased risk for BRCA-related cancer."
