The Reason Our Hospitals Are Failing Rape Victims

By:
Victims of sexual assault can potentially face countless obstacles in the criminal justice system, from local police stations to the court rooms where their attackers are sentenced — if they end up getting prosecuted at all. 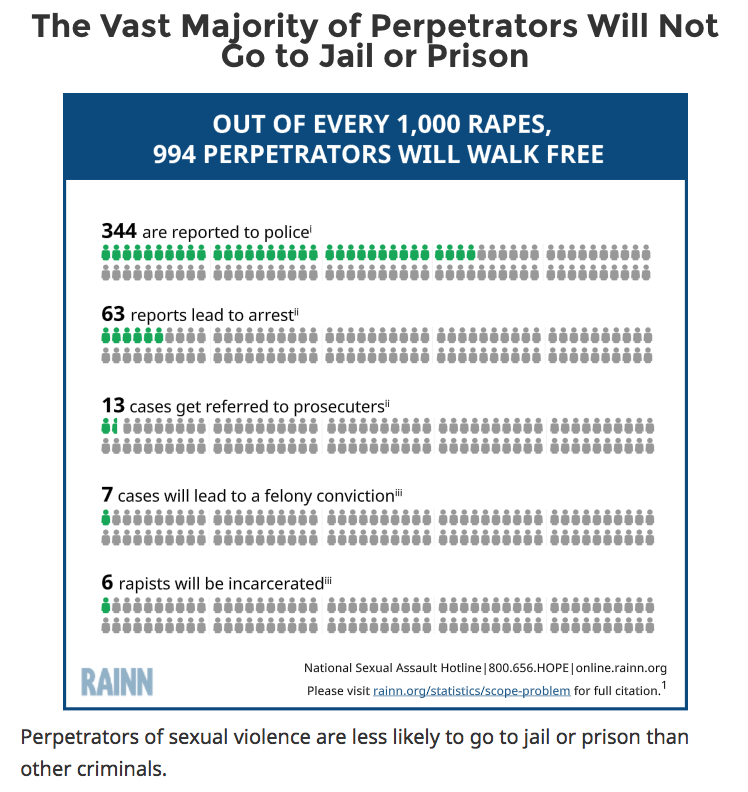 RAINN - rainn.org
RAINN - rainn.org
But many hospitals in the U.S. also are failing rape survivors, according to a May report (PDF) from the Government Accountability Office.
 AP/Pat Sullivan - apimages.com
AP/Pat Sullivan - apimages.com
Though states can receive federal funding to train sexual assault nurse examiners (or SANEs), they often fail to do so or even provide data on these programs, the report concludes.
SANEs are often one of a victim's first points of contact after a sexual assault, and they serve a crucial and complicated role.
In addition to conducting medical exams, documenting injuries, and performing a rape kit collect DNA evidence, they also provide psychological support to victims in vulnerable moments, Broadly explains.
 AP/Pat Sullivan - apimages.com
AP/Pat Sullivan - apimages.com
SANEs are trained to cooperate with police investigations, follow the chain of custody of evidence, and can be called to testify in court about their findings.
Hospitals are understaffed with SANEs across the United States.
From the GAO report:
"In 49 states, approximately 227 grantees or subgrantees—referred to collectively as grantees—reported providing training for over 6,000 examiners in 2013. The type of training examiners received ranged from comprehensive examiner training to training on specific topics, such as courtroom testimony. The extent of examiner training efforts supported with funds from the three DOJ grant programs varied by state. For example, in about half of the states, fewer than 100 examiners received training. In addition, in the states where at least one grantee funded examiner staff positions in 2013, grantees funded less than one position, on average."
Rural areas came up especially short-staffed.
Almost half of the counties in Wisconsin had no examiners available. Though the state "trained 540 examiners over a two-year period, only 42 of those examiners were still practicing in the state at the end of those two years," the GAO reports.
Even in hospitals with trained SANEs, examiners were often on-call and not available around the clock.
It isn't required by law that sexual assault victims receive exams by SANEs rather than other nurses, Terri Slapak-Fugate, the Director of Emergency/Urgent Care and the SANE Program Manager at Southwest Health Hospital in Platteville, Wisconsin, explained in a May Washington Post op-ed.
Slapak-Fugate described how her experiences dealing with sexual assault victims as an emergency room-nurse first led her to seek out SANE training and become certified in 2014.
"I would try to make sense out of the rape kit: a cardboard box packed with numerous envelopes holding a mess of long-handled swabs and slides. Instructions were printed on both sides of a sheet in type so small I could barely read it. Often, the doctor on call was as uncertain about what to do as I was and had only 10 or 15 minutes before needing to return to other emergency department duties. I felt inadequate to meet my patients’ needs. And I was always worried: 'What if I mess something up in the rape kit and ruin her court case?'"
A 2003 study on Colorado rape kits published in the Journal of Emergency Nursing found that a large number of rape kits did not collect the proper number of swabs (29 percent), were sealed incorrectly (25 percent), or did not follow the chain of custody required by law enforcement (19 percent). The kits conducted by SANEs were much less compromised — only 12, 9, and 8 percent of kits included these particular errors.
In an interview with Broadly, International Association of Forensic Nurses' interim CEO and education director Jen Pierce-Weeks delved into some of the reasons she believes there is such a shortage of SANEs.
"I believe vicarious trauma contributes to nurses not staying in the work because oftentimes it is not taken seriously, nor recognized when it is occurring," she told Broadly.
She also said that hospital administrators did not always "devote the resources necessary to support ongoing SANE services," and cited a belief among healthcare professionals that SANE programs should be "a social and criminal justice issue."
"This leads them to believe it is not health care's duty to respond," she explained. "This also leads them to believe SANE is an 'arm of law enforcement,' when nothing could be further from the truth."
Senate Democrats introduced a bill in May — the Survivors' Access to Supportive Care Act — that would expand SANE training programs and require more oversight.
“When survivors of sexual assault seek medical care they should be offered the best information, services, and support available,” Sen. Patty Murray (D-Wash.) said in a press release. “Unfortunately, many states and hospitals are failing to provide survivors with access to quality care that is critical to their recovery and to holding perpetrators accountable. I’m proud to be introducing legislation that would help develop standards of health care and training in hospitals and medical settings nationwide, and I’m committed to continuing to push for better access and higher quality care for survivors of sexual assault in Washington state and across the country.”
