Why Mental Health Is So Hard to Diagnose

By:
Approximately one in five adults is affected by mental illness nationwide, but many factors may complicate the ability of patients and mental health professionals to solidify a diagnosis before treatment.
It’s difficult to know how many mental health disorders are misdiagnosed — especially when considering both over and and under diagnosis. In the case of some mental disorders, initial rates of misdiagnosis may affect more than half of all patients. Research suggests that over 70 percent of the 5.7 million people affected by bipolar disorder initially receive an incorrect diagnosis, and one study has suggested that as many as one million young people may be misdiagnosed with attention deficit/hyperactivity disorder.
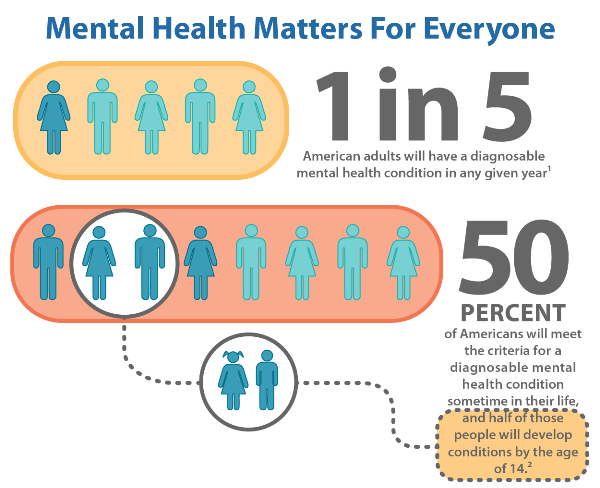 Mental Health American of the Heartland - mhah.org
Mental Health American of the Heartland - mhah.org
Symptom similarities make diagnosis particularly difficult.
Many factors contribute to the misdiagnosis of mental health, despite the best efforts of mental health professionals. Psychiatry is an exceptionally challenging field. The fact that much is still unknown about the brain, paired with the reality that many different psychological disorders exhibit similar symptoms, can make the diagnosis of psychiatric disorders very difficult.
“We have the issue of this heterogeneity and trying to map it onto symptoms that sometimes sound similar across different disorders,” Dr. Sherry Ann Beaudreau, a clinical associate professor at Stanford University School of Medicine, explained to ATTN:. “Because of all of the heterogeneity and the fact that these disorders were put together…. more by critical observation, the time has come where that’s changing and it’s being looked at differently.”
 American Foundation for Suicide Prevention - afsp.org
American Foundation for Suicide Prevention - afsp.org
In the face of this challenge, research organizations such as the the National institute of Mental Health are working to develop creative solutions to approach mental health from multiple angles. RDoc, a new research framework launched by NIMH in 2014, works to combine the many levels of information, from the most technical levels of genetic study to patient support, to better understand human behavior, including psychiatric disorders.
“...let’s try to look at what the brain actually does and what’s important and what the major systems are, and explore that and try to mental disorders in those terms,” Bruce Cuthbert of the NIMH explained in a video introduction to the program. “...rather than making these symptom categories and assuming that the problems in the brain and the problems in behavior should line up one to one with these categories that were defined in complete absence of any knowledge about the brain from 100 to 2,000 years ago.”
Mental disorders may be masked by physical ailments, and visa versa.
Connections between the brain and body are still being uncovered, but a marked relationship between medical and psychological symptoms may contribute to diagnosis difficulty in both disciplines, with one study suggesting that at least 10 percent of psychological symptoms may be driven, first, by a medical condition.
In other cases, Beaudreau said, psychological issues may exacerbate medical symptoms, such as gastrointestinal issues or heart palpitations in the case of anxiety.
“It’s always this balancing act, trying to figure out whether symptoms are a part of a psychiatric disorder or are part of a medical condition,” said Beaudreau to ATTN:. “And sometimes it’s both, and sometimes patients think it’s a medical disorder, but it’s actually part of their anxiety or depression disorder. So I think we walk a really fine line trying to figure that out.”
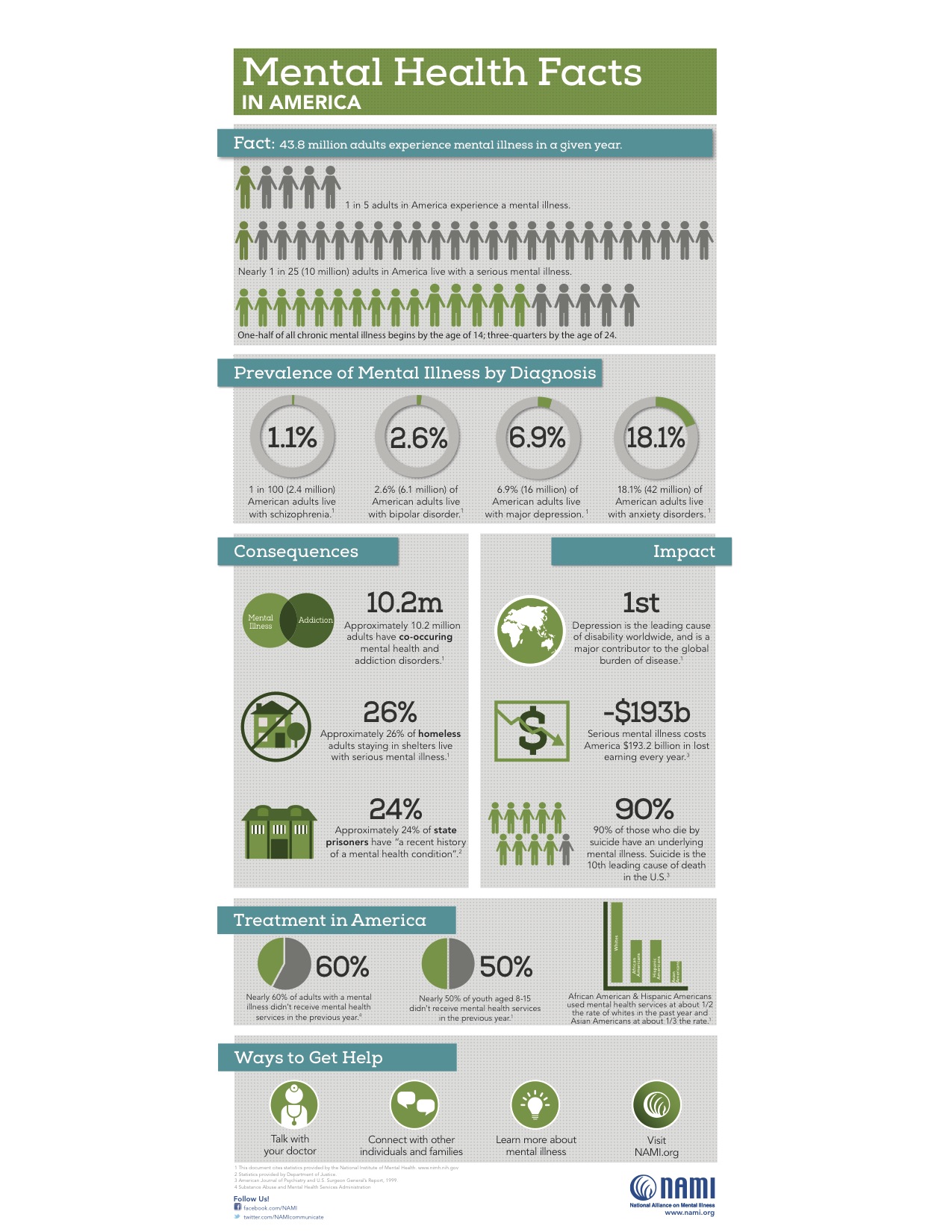 National Alliance on Mental Illness - nami.org
National Alliance on Mental Illness - nami.org
And as is the case with physical medicine, mis-reporting, missing history, and stigmas can also inhibit a successful initial diagnosis.
According to a study from the University of Chicago, some people who may benefit from mental health services fail to seek treatment due to the social stigma surrounding mental health. Ability to access mental health services may also hinder treatment, with more than 56 percent of adults with a mental illness failing to receive treatment services, according to Mental Health America.
But a growing number of resources are available to individuals seeking mental health treatment and support.
The National Alliance of Mental Illness provides free, 24/7 crisis text and call support, and Mental Health America provides resources for finding online support groups, screening tools, and assistance in finding mental health care services. If you are concerned about your mental health, but do not have a mental health support team in place, consider speaking with your primary care physician.
