Judge Rules Against Force-Feeding Terminally Ill Anorexic Woman

By:
On Monday a New Jersey state superior court judge ruled that a 29-year-old woman terminally ill with anorexia has the right to refuse force-feeding treatments, the Wall Street Journal reports.
The woman, identified as A.G., was hospitalized in a state psychiatric ward for more than two years after a life-long battle with anorexia.
The judge granted her request for palliative care, a medical technique that aims to provide comfort (rather than aggressive and arguably oft-futile treatments) to terminally ill patients.
The case traces back to a court order A.G.'s court-appointed temporary guardian received in June.
The order mandated A.G. be force-fed through a feeding tube at Morristown Medical Center, the Daily record reports. Leading up to the ruling, her weight fluctuated between 60 and 69 pounds.
Though the feeding regimen resulted in a weight gain of roughly 30 pounds, it also triggered heart failure due to "re-feeding syndrome," fatal shifts in fluids and electrolytes that occur when malnourished patients receive food. A.G. subsequently pulled out the tube herself.
The state opposed the decision, saying it was tantamount to state-assisted suicide, according to the Science of Us.
"The state argued that her depression renders her unfit to make her own medical decisions and that no longer force-feeding her is sanctioned suicide; they want to treat her depression with an experimental course of ketamine. Her doctors testified that she’s been diagnosed with late terminal anorexia-nervosa and isn’t likely to recover. Her psychiatrist said that force-feeding would be 'cruel and torturous at this point,' as she has the bone density of a 92-year-old and restraining her to insert a feeding tube through her nose and down her throat could break her bones. And, as her court-appointed lawyer argued, force-feeding would keep her alive but would not treat her anorexia."
Palliative care typically comes up in terms of elderly patients and is controversial even within that context.
In 2014, approximately 84 percent of hospice patients were 65 years of age or older—with 41 percent being 85 or older, according to the National Hospice and Palliative Care Organization. The same report estimates that 63 percent of care is for non-cancer diagnosis including heart disease, dementia, and lung disease.
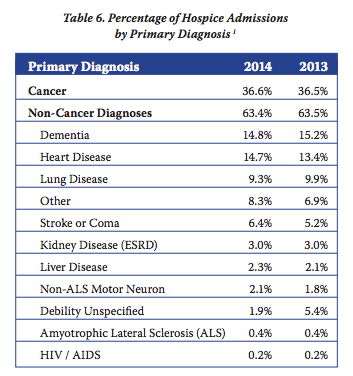 National Hospice and Palliative Care Organization - nhpco.org
National Hospice and Palliative Care Organization - nhpco.org
But even in the phase of life when death looms nearer, there are reservations. As Anemona Hartocollis wrote in the New York Times, "As an aging population wrangles with how to gracefully face the certainty of death, the moral and economic questions presented by palliative care are unavoidable: How much do we want, and need, to know about the inevitable? Is the withholding of heroic treatment a blessing, a rationing of medical care or a step toward euthanasia?"
The medical ethics of palliative care are further complicated when mental illness is involved.
This debate recently surfaced when a woman in the Netherlands was euthanized for incurable PTSD due to sexual abuse, the Independent reported.
Though these cases differ in important ways, both illuminate the difficulties of negotiating boundaries between mental illness and physical illness. Successful patient care will require balancing individual patients' needs with a desire to encourage others to combat mental health issues through therapy, medication, and other means.
